Obesity rates in the United States are the highest in the world and a growing health concern. In fact, according to data published by the Centers for Disease Control, 67% of men and 62% of women are overweight. Thirty-four percent of women and 28% of men could be further classified as obese. It’s a contributing factor in numerous diseases like Type 2 diabetes, cancer, stroke, and coronary artery disease.
Because obesity puts patients at greater risk for a host of other medical conditions, they’ll ultimately require more tests and scans during their lifetime in comparison to leaner patients. When it comes to nuclear imaging, obese patients and the unique challenges their weight presents can further hinder an accurate diagnosis and an optimal treatment plan.
Imaging and obesity-related challenges
Consider something as simple as diagnostic testing. Most nuclear cameras are designed to accommodate the standard, ideal-weighted patient. With obesity rates climbing at an alarming rate, physicians need to think about whether their equipment can adequately serve this growing population.
Many of today’s SPECT cameras still have a maximum weight capacity of 250-300 pounds. This standard feature can make imaging impossible for larger patients and can put both the patient and the technologist at risk.
For example, an obese patient will have difficulty getting up on, positioning and balancing themselves, and remaining still as they lay on a standard imaging table. They’ll also have to turn over or step down from the table, which could be equally as dangerous. Obese patients have a different center of gravity, which is a significant safety concern that needs to be addressed.
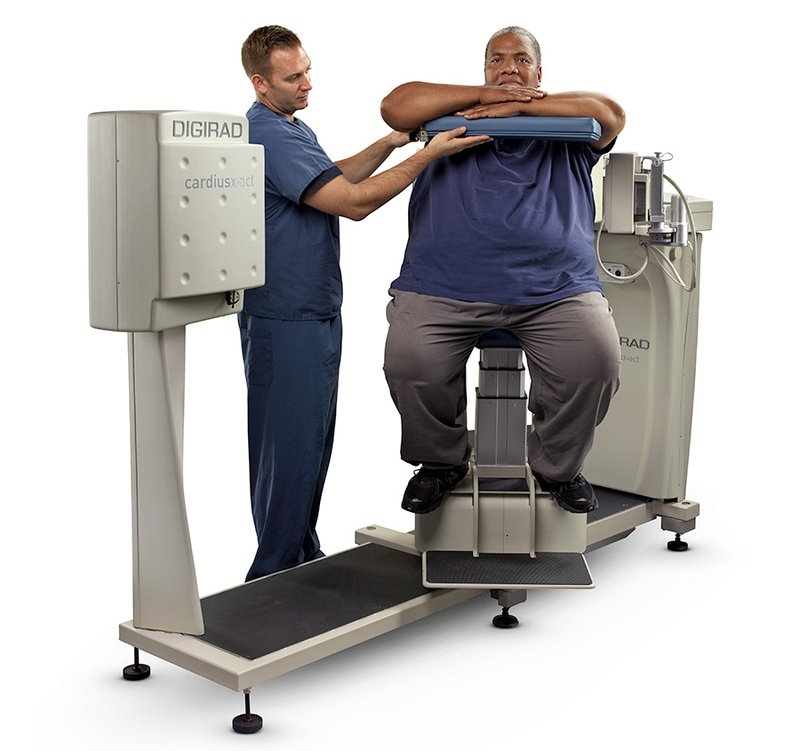
Some SPECT cameras, like the Digirad X-ACT+, utilize the more patient-friendly, seated position, which all but eliminates the patient’s risk of injury from climbing up on, balancing, turning, and stepping down from a supine-positioned table. It also has a maximum weight allowance of 500 pounds, a larger gantry for ingress and egress, and handrails for support.
Orbital space, girth, and field of view
Another issue is reduced orbital space. If the distance between the patient and the detectors is not sufficient, the detectors may not be able to rotate properly. Especially when imaging larger patients, the risk of truncation occurs if the detectors are not able to clear the distance, or cover the girth.
Many of today’s SPECT cameras also have a fixed detector design, which challenges the ability to position the heart of an obese patient in the “sweet spot.” A leaner patient’s heart is more likely to be ideally positioned because today’s cameras are designed for their average body type.
With any size patient, a technician should be able to center the heart in the field of view with relative ease, like with the Digirad X-ACT+ camera. Once the patient is seated, the chair can be moved forward and backward and from left to right in order to optimally position the heart inside the field of view and with enough distance from the detectors.
Attenuation, radiation, and scan time
Images with excessive attenuation and scatter are also more prevalent with obese patients. Dense breast tissue, for example, in both male and female patients, makes it more difficult to acquire accurate quantitative information. Attenuation correction has significant diagnostic value for all patients, but especially obese patients. With it, image clarity and quality are improved, which can result in fewer false positives and fewer unnecessary cardiac catheterizations.
Radiation dosage and scan times for obese patients can be an issue too. While there are standard imaging protocols, they were created for an average weighted patient. Dosage calculations are higher and scan times are longer for obese patients, but those estimated amounts can miss the mark. A low estimate compromises the quality of the images and a high estimate unnecessarily increases the radiation burden to the patient.
The Digirad X-ACT+ camera not only performs attenuation correction with a radiation dose of less than five microsieverts, it also uses TruACQ Count Based Imaging™ software to calculate dosing and scan times. Without the guesswork, technologists can proceed with confidence and ultimately work to deliver higher quality images.
Many of the imaging problems that accompany obese patients can be overcome with the right equipment and software. In reality, though, technicians and cardiologists will simply work with the equipment they have to do the best job they can. At Digirad, we believe that every patient deserves the highest quality of care, regardless of their weight.
Digirad can help
The fact that an imaging system can easily accommodate obese patients may not be the sole reason you choose a camera. However, when that benefit is paired with state-of-the-art technology that can help deliver a higher level of quality of care for a broader group of patients, it’s hard to ignore.