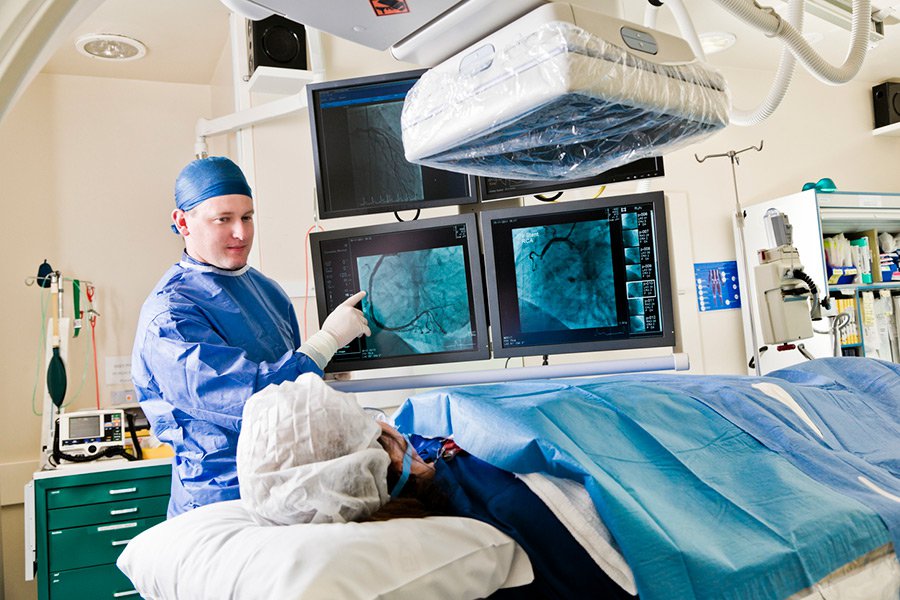
Cardiac catheterization is one of the most common diagnostic procedures for heart patients. But, because of its invasive nature, it can carry a higher risk of patient-related and procedure-related complications.
These complications can often lead to hospital readmissions which, under Medicare, not only serve as a performance measurement for hospitals and physicians, but also incur a steep financial penalty if they occur within 30 days of the procedure.
How do hospitals that are continually looking for ways to cut costs, and physicians who are trying to find the most direct route to a solution work together to reduce the risk of readmissions? In this post, we’ll explore different ways to reduce readmissions rates and make the procedure better for everyone involved.
Take a non-invasive approach
Non-invasive techniques offer lower risks for complications and can be used to ultimately confirm or negate the further need for cardiac catheterization. By following appropriate use criteria (AUC) and leveraging tests like FFR, SPECT MPI, Attenuation Correction SPECT MPI or PET imaging, cardiologists can potentially perform fewer unnecessary procedures, a benefit to both the patient and the healthcare system.
Integrating AUC compliance into clinical care will also help collect data that physicians can use to design the most appropriate treatment plans and deliver improved clinical outcomes.
The bottom line is that a non-invasive approach that can help physicians formulate a more confident clinical decision should be the first line of defense. While it may ultimately lead to an intervention, it could also avoid the assumption of unnecessary risks. By substituting technology with higher accuracy such as Attenuation Correct SPECT MPI or PET MPI, a large number of normal patients will never have to undergo a needless cardiac catheterization procedure.
Reduce the risk of complications
When cardiac catheterization is the most appropriate treatment, it’s critical for the hospital staff, physician, and patient to be intentional about reducing the chance of complications, and therefore, readmissions.
Many factors can influence a patient’s likelihood of developing vascular complications during or post procedure. They include individual patient characteristics, the cardiologist’s technique, the choice of either manual or mechanical compression at the access site, the medications used during the procedure, whether a closure device was used, and the quality of postoperative nursing care the patient receives.
Complications can range from minor issues without long-term effects to major problems that require emergency care or surgical intervention. Here are some ways to minimize the chances of complications either before, during, or after cardiac catheterization:
1. Identify patients at risk
Assessing a patient’s risk level begins with their medical history and current state of health. Elderly adults, patients with renal failure, and women, in general, have a higher risk of vascular complications. Obese or extremely thin patients are more prone, as are those who have severe peripheral vascular disease or severe systolic hypertension.
Patients with a low baseline hematocrit level and platelet count, or who have congestive heart failure, chronic obstructive pulmonary disease, or coagulopathy also assume an elevated risk level. Recognizing the risk factors up front and identifying patients who fall into these categories will put you on higher alert for specific signs and symptoms.
2. Choose the most appropriate approach
Radial catheterizations are generally considered to be easier on the patient and more comfortable, too. It’s a smaller artery that, with applied pressure, stops bleeding more easily.
Patients can walk around, leave shortly after the procedure, and return to normal activities, like walking and driving, sooner than others. Recent clinical trials associated the transradial approach with lower risks of bleeding and vascular complications as a whole.
With the femoral approach, patients are required to stay in the hospital on bed rest for a few hours with greater limitations upon discharge. Movements by the patient, such as bending legs or ambulation, can lead to bleeding and coupled with the use of anticoagulation therapy, the risk is even higher.
Clinical trials have also supported the assertion that the location and the size of the femoral artery makes bleeding more likely and more difficult to manage in comparison to radial catheterizations.
3. Maintain homeostasis
Maintaining homeostasis at the access site until the bleeding has stopped will reduce complications, increase safety and comfort, and shorten a patient’s hospital stay – another win for the patient and the healthcare system.
Generally, manual compression is very effective, but depending on the size of the sheath placed in the artery, it may take between 10 and 15 minutes of direct pressure, sometimes even longer, to stop the bleeding. As an alternative, you can use a vascular closure device, which will seal the puncture immediately.
4. Use anticoagulants
Pharmacology plays an important role before, during, and after cardiac catheterization. Since thrombosis is one potential complication among cardiac catheterization patients, antithrombotic prophylaxes have proven to be especially effective. The surgical staff should be well versed in anticlotting medications, their drug classification, mechanisms of action, correct dosing, and potential adverse effects.
5. Premedicate patients with known allergies
The use of contrast in cardiac catheterizations can also lead to complications like allergic or anaphylactic reactions and nephropathy. Patients with seafood, penicillin, or atopic allergies, or those who have suffered past adverse reactions are at a considerably higher risk.
You can, however, decrease the likelihood by premedicating these patients with glucocorticoids, H1 antihistamines, and H2 antihistamines. Ionic contrast should also be avoided and replaced with low- or iso-osmolar nonionic contrast.
6. Provide high-quality post-procedure care
Following cardiac catheterization, patients generally require several hours for recovery and are then transferred to a hospital or outpatient room. Many of the typical complications present themselves during the transition, which means the staff must be even more vigilant post-procedure.
Most complications are caused by inconsistencies in patient assessments, medication errors, unrecognized changes in a patient’s condition, unintentional sheath removal, and a lack of appropriate intervention.
Studies show that meticulous postoperative care performed by critical care nurses contributes significantly to a successful recovery void of complications. Vital signs should be taken every 15 minutes for the first hour, every 30 minutes for the next hour, and then every hour moving forward. Symptoms, mental status, blood pressure, and respiratory status should be continually assessed until the patient is discharged.
To ensure a consistent approach to care, a hospital’s administrative and nursing leaders should consider developing protocols and policies for patients who undergo cardiac catheterization.
Many facilities provide educational seminars and simulation labs on site, and to improve safety and care, have established specialty units exclusively for cardiac catheterization patients.
The bottom line
Cardiac catheterization, like any other invasive procedure, will always pose a higher risk for readmissions. With the reliability of alternate, non-invasive studies, clinical decision-making can help avoid potential readmissions. But, when cardiac catheterization is indicated, there are multiple precautions that can mitigate complications and ultimately reduce readmissions and their financial consequences.