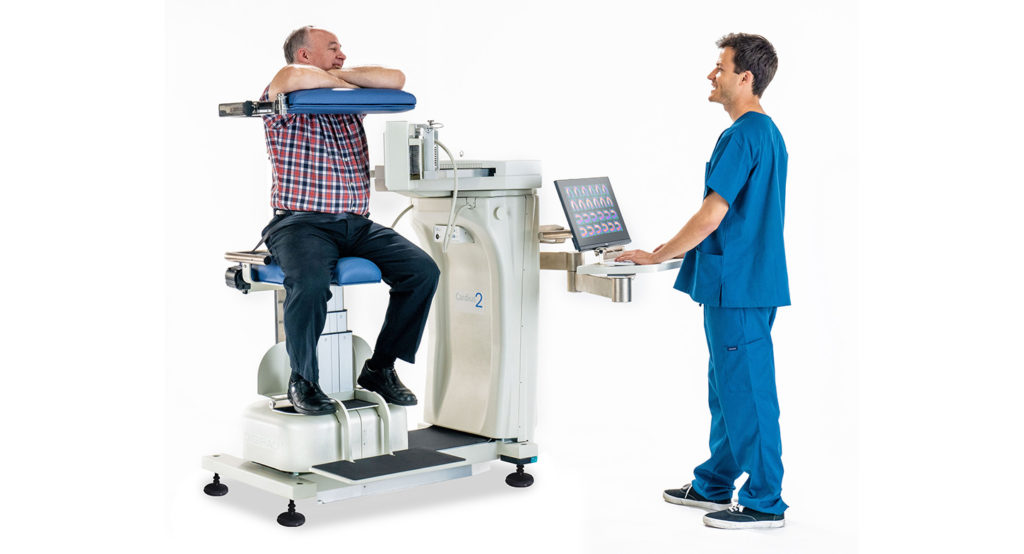
Although performing a SPECT MPI study in the supine position is common, upright cardiac imaging continues to gain in popularity. While the study type and camera technology are similar, the physical position of the patient affects critical aspects of both the study and the image. In this post, we take a look at the differences between supine and upright cardiac imaging.
1. Body Position and Image Quality
The position of the patient during a cardiac scan can affect image quality. When a patient is lying down, the position of organs and tissue shifts and can result in unwanted artifacts.
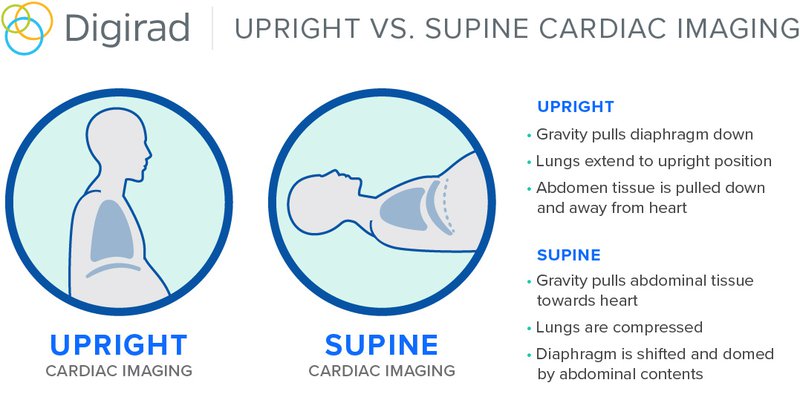
When a patient’s arms are raised in the supine position, it can cause the diaphragm to move, which may obstruct a clear view of the heart. Additionally, it’s common for breast tissue to shift when the patient is supine. When performing a SPECT MPI study, the breast tissue can cause unwanted artifacts if the scan is done in a supine position.
Upright imaging offers the benefit of allowing the technologist to center the heart in the field-of-view without extending the torso, thus keeping the diaphragm or breast tissue lower and reducing the potential for artifacts.
As ASNC President Sharmila Dorbala, MD, MASNC, stated in the Harvard Health Letter, “The upright imaging position helps because gravity pulls the stomach and the intestines down a little bit and out of the way of a clear view of the heart.”
2. Patient Comfort
With supine imaging, the patient climbs onto and positions themself on a roughly 15-24” wide imaging table. Face-up, they lie still with their arms raised above their heads, which can be uncomfortable for patients with COPD, arthritis, or other shoulder or arm impediments.
The size and the location of the camera detectors also have the potential to exacerbate any feelings of claustrophobia since they rotate so closely around the patient’s face or chin.
The general consensus among patients is that if you can comfortably get in and out of your car, you can get up and down from an upright imaging gamma camera.
The patient’s arms rest on the device’s armrest, which alleviates the need for the patient to stabilize that overhead weight. The seated position is easy to navigate, and the more compact detectors are less imposing, which offers a significant improvement in comfort and patient anxiety.
3. Interpreting the Exams
Due to differences in the anatomic distribution of potential sources of artifacts, quantification of the two methods will vary by gender and by imaging convention (upright or supine), so a parallel comparison is vital.
Supine patient studies should be scored against a normals database created with studies acquired on a supine system; upright patient studies should be compared to a normals database created with studies from an upright system.
When using a normals database for comparisons, one must be certain to use a database of true comparables with regards to these variables. The normals database should include separate images for male and female anatomies.
Which is a Better Choice?
Clinically, either position can result in quality cardiac images that provide diagnostic confidence. However, due to anatomical structures moving, incidental attenuation, and overall patient comfort, upright cardiac imaging has key advantages over supine imaging. Additionally, the preference revolves around comfort and ease of use from both the patient and the technologist’s perspective.
In today’s healthcare marketplace, where quality of service can be directly correlated with patient satisfaction, retention, and referrals, upright Myocardial Perfusion Imaging is gaining support in the broader imaging community.